 Clear birth tub at The Birth Center of NJ. Clear birth tub at The Birth Center of NJ.
Below is a database of waterbirth tubs and labor tubs in northern NJ for those researching options - sometimes referred to as aquatherapy or hydrotherapy (please click on the individual record to open the image link).
As you can imagine, water is wonderful for creating more buoyancy for the birthing person. Another added benefit is that is creates a little bubble of a birthing space for the birthing person. Places with the most options include: The Birth Center of NJ and Our Birthing Center and Morristown Medical Center. Please note that some of the hospitals will say they have waterbirth tubs, but they may ONLY have inflatable tubs that rarely see the light of day.  Celestial skyscape overhead at The Birth Center of NJ. Celestial skyscape overhead at The Birth Center of NJ.
Also, please note that if you wish to birth in a hospital tub, you will need to check with your provider if they will catch your baby in the tub or will want you on the bed for the actual delivery. Oftentimes, the birthing person does not think they want to birth in the tub, but then regret not lobbying for the option, because they felt disturbed having to get out of their birthing space in the tub (something to think about and chat with your partner and doula about).
In addition to the Birth Centers and Hospitals, Homebirth is another wonderful option for waterbirth and many people arrange to have an inflatable tub brought into their home. Feel free to get in touch with Rachel (via the contact page) if you have any questions or want her to find more info for home, hospital, or birth center. Good luck researching your waterbirth options!
Instructions for Database:
- Click on record to see more info. - Scroll down to view all records. - Send us any updates. Thanks!
If you have updates to this database or have updated links for images, please let us know. Thanks!
3 Comments
Not everything comes naturally but that is no reason to be discouraged from pursuing something you want to pursue.
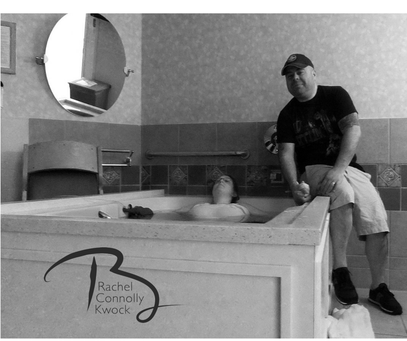
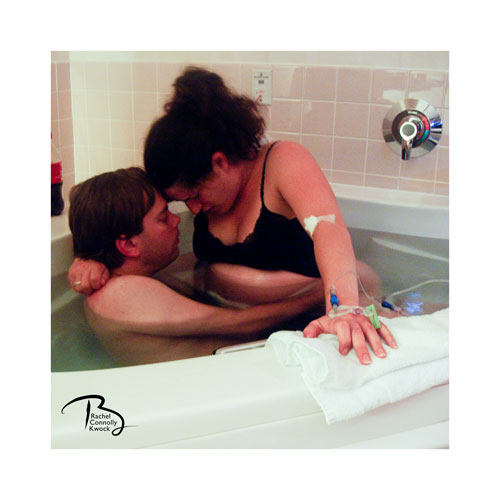
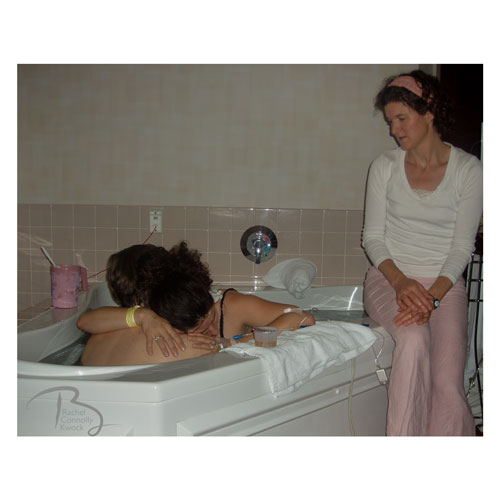
Sometimes we need to learn the basic skills first in order to feel comfortable enough to let our intuition really flow and to allow things to come naturally – to have the ability to “just know” something without any proof or evidence. Take a chef for example – to be able to say “oh I just added a touch of this and stirred in a little bit of that” is usually from years of trial and error – from souring sauces and burning side dishes. Now they can play around with seasonings. Or consider a businesswoman who says, “I followed my gut” or “I had a hunch about that deal” – it’s often from years of experience and observing behavior, analyzing metrics, and taking risks. They already know how far they can push things and what the likely outcome will be. Intuition as a learned skill applies to business and creative pursuits as well as many of other vocations – and in my personal experience, it applies to working as a birth doula in northern New Jersey. As a birth doula, a woman who supports and serves women in childbirth, it was frustrating when I started to have more-experienced doulas tell me – “just to follow your intuition”. I would think–I have no idea where this intuition, you speak of, starts or where it leads, so can you please provide me a little direction? When I started as doula, I would always do a simple hip squeeze – placing my hands on either side of mom’s hips, applying pressure to relieve pain and tension. I did this repeatedly because neither my skills nor intuition was guiding me anywhere else. About a year ago I participated in a workshop where we learned in-depth information about positioning for mother and baby and am now able to follow my intuition more. The workshop changed by practice. Knowing more helped me be more intuitive. Now when I support a mother – I know to breath out any tension and let any thoughts go from my own mind – to leave the suitcase at the door. I listen to what comes intuitively - to the sounds of the birthing space and the birthing woman. Tuning in helps me listen to the sounds of her movements – whether they be tired, tense, relaxed, imminent. I can sense her clenched jaw and gently rub her jawbone to provide release. I can tell she is hold tension in her pelvic area by how she paces and positions herself during contractions – and can gently place my hands on her sacrum to offer her release and support. Are her legs tired from standing all night? I can feel if her muscles are taught or wilted and go on to provide a gentle foot massage or little wiggle to shake out her lax limbs. It took me years of building my knowledge and skills to get to the point where I felt I could follow my intuition but now I feel confident to enter the space of a birthing woman and close my eyes and listen to the space and to what her body is telling me – where her body is guiding my hands to go, to be intuitive. To “just know.” So if this skill of intuition was there all along and is available to all of us - how can we hone it? How can we simply be more attuned and responsive to the subtle clues we receive? Scientific America Magazine wrote that intuition is linked to the basal ganglia area of the brain – an area that controls fast, automatic, cognitive operations. So it would make sense that to hone our intuition we need to improve or maintain our brain health. As many studies show – brain health can be maintained with good diet, exercise, plenty of sleep, and clearing the mental clutter. To be a good listener and more intuitive, it is important to turn off the chatter in our brains. We can do this using meditation or periods of silence and solitude where we focus on our breathing or something that brings us peace. In order to be better listeners in our environments, we need to turn off the noise. So intuition may not be a mystical thing for all of us. If we are experts or even very experienced in our fields – it may be a matter of just connecting the constellation of silent clues we receive in order to yield an intuitive response. Being intuitive can be a wonderful, freeing feeling. I will never, ever say to a doula starting out – “oh just follow your intuition” as if they already have that roadmap. For some of us, it is only possible to follow our intuition after we have created a map that charts skills, knowledge and experience. Only then can we can paint with broad brush strokes of intuition over the charted ones. As Picasso says, “It took me four years to paint like Raphael, but a lifetime to paint like a child.” Fellow doulas, what helped you to follow your intuition more? Photo shared with permissions. PC: Rachel Connolly Kwock. Feat.: Doula Holly Graff & Midwife Donna Tabas.  (Republished in honor of Midwives of NJ Symposium. Original story from July 5, 2009) Sometimes we here at Birth POV have the privilege of publishing a birth story- this is one of those times.... In 2009 I was so honored to be invited into Jennifer and David's life to attend my first birth as an apprentice doula- it was very exciting! Thank you Jennifer, David, and Jacob for letting me share your story here. This was originally written for DONA evals so there are a lot of little details. Thursday afternoon, Jennifer and I spoke on the phone. She had an appointment that morning and was found to be 1.5 cm dilated, 50% effaced, and -2 station. She felt like maybe the exam had gotten things moving a bit because she was feeling a little crampy and was spotting. I made sure all my bags were packed. Friday morning Dave called around 8a to say the contractions were 2-3 minutes apart and they were probably going to hospital that day. I showered, left the kids at daycare, and headed due west on route 80 to Hackettstown Regional Medical Center. I arrived at the hospital at 10am and was scooped up by Dave & Jennifer as they were driving in, “you wanna’ get in?” I loaded in my bags and body on top of their bags and we headed up the hill to the hospital. We all went in – a passer-by said “what a wonderful day for you” to Jennifer. Jennifer ambled up to the receptionist and said “I’m having a baby” All the ladies behind the desk laughed. “I’m in labor, right? This is labor right? “They took all Jennifer & Dave’s information and sent us upstairs. We had so many bags between us that we asked the newspaper delivery guy to help us with his cart. He seemed happy to do so. Jennifer kept saying that she thought she brought too many towels. We unloaded all our belongings onto the floor of the labor room, specially designed with a waterbath for birthing - one of the only facilities in northern New Jersey. The midwives (Lisa Lederer CNM of Midwives of NJ and apprentice midwife Karen) came in and listened to Jennifer as she caught them up on her laboring and how she’d been laboring all through the night and not getting any rest. Jennifer was indeed in early labor but since she laughed her way through every statement the midwives joked they didn’t believe she was in labor if she was laughing so much. At 10:30 am they examined Jennifer but said she was only 3cm, 75% effaced, station –2. They also said they thought the baby was a little right occiput posterior so it was kind of looking front and to the side a bit, instead of directly back. They suggested Jennifer go home to labor or walk across the street. Jennifer wanted to stay in the room and hospital but Lisa said “there’s nothing magical about our hospital - babies don’t come out just because you’re here!” Besides, the midwives said the moms tend to walk around the corridor and then just want to come back in and lie down in the bed, which doesn’t help labor progress. We all wanted to go outside but didn’t want to move all the bags again! The hospital agreed to hold the cordblood banking kit but we had to take the rest. Moving all the bags seemed like a drag but leaving seemed like a good idea – worth moving all the bags for. I was grateful that the midwives told us to go labor elsewhere and let things transpire naturally rather than start intervening so early in the labor. Once we got outside, I asked Jennifer if she could start walking thru the contractions and she did. Jennifer felt defeated and embarrassed at being asked to labor elsewhere. I asked her if she could let go of that and without pause, she replied, “yeah! I can let go of that.” We walked down the hill surrounded by blue skies and green mountains. Dave knew of a café at the bottom of the hill where he suggested we eat lunch.  At the bottom of the hill, we walked across the street to the Willows – a cute little café run by a German woman who was very excited to have a woman laboring in her café! She sold us on the “German fries,” which were basically like hashbrowns, and her helper made us some chicken wraps that Dave and I ate. Jennifer didn’t have the stomach for much but ate a little chocolate and drank some water. What Jennifer really had a palette for was the monstrous plate of berries the owner brought to her! Blueberries, raspberries, and a peppermint leaf to top it off, which Jennifer would sniff repeatedly throughout the afternoon. She found the peppermint smell soothing during contractions. Eventually we dumped all the berries into a cup, said goodbye to the Willows Café and took our berries on the road where they acted as the little inter-contraction treat. Arm and arm with Dave, Jennifer pushed herself to walk thru her contractions – pushing herself a little more all the time. Berries, sniff of mint leaf, uh-oh here it comes again, hold onto Dave, hold onto Dave, hold onto Dave, okay it is going away now. In addition to being there for Jennifer to lean on, Dave was also busily timing the contractions with his device. Jennifer and David figured out they had been mistiming the contractions in the morning and that is why they thought they were further along than they were. They now had it down to a science and the contractions really were 2-3 minutes apart! So with Jennifer contracting and eating berries we walked down the street. No outlet - turn around, thru the development – too hot, into the midwives' offices – the midwife says keep moving and roll those nipples, into the car – "sitting is horrible!" Short ride to Stephen’s Park, a beautiful shaded park with a river gushing through. Dave suggested the park and it was a great idea because it was cool and shaded and semi-private so Jennifer could roll her nipples without an audience. There was one group of kids there who looked a bit curiously on us when I was bent over like a triangle trying to do a double hip-squeeze on Jennifer while she was moaning and groaning her way through a contraction but they kept walking. I massaged Jennifer for a little bit until we decided to take a walk down one of the paths to an island Dave knew of. Walking down the path, Jennifer pushed herself to walk and sometimes stopped to just hang onto Dave.  When mom arrived at the hospital, she wasn't in active labor. The midwives wanted her to go out for a walk. Mom wanted to stay in the l&d room , but the midwives said "There’s nothing MAGICAL about our hospital - babies don’t come out just because you’re here!” Mom went for a walk. When mom arrived at the hospital, she wasn't in active labor. The midwives wanted her to go out for a walk. Mom wanted to stay in the l&d room , but the midwives said "There’s nothing MAGICAL about our hospital - babies don’t come out just because you’re here!” Mom went for a walk. Her contractions were building. The walking and nipple stimulation seemed to be helping. We crossed over the bridge to the island. Jennifer used the bridge as support to push and pull against - balancing on bridge rail. It was here that Jennifer found her yogic ohm sounds that helped her through this part of labor. We hoped the technique would open things up – ode to Ina May and the Sphincter concept. It was a beautiful thing watching Jennifer and Dave on the bridge – Jennifer’s voice a clear and present ohm. Jennifer and David so affectionate and loving with one another – kind of in a slow dancing position, intertwined on the bridge in a contraction wave. Who knew labor could be so peaceful? This was a really special time during the labor. We spent a long time there on the bridge with Jennifer ohming, eating berries, sniffing the peppermint leaf, taking pictures. Eventually the berries became overly ripe and Jennifer was ready to move onward. We walked back to the picnic table where we did the double hip-squeezes and I suggested Jennifer get in the hands and knees position for a little while I did some effleurage, but wasn't sure if I was supposed to be gently coaxing the baby the right direction or kind of pulling it, so as a novice doula, I went with gently coaxing. Jennifer was such a good sport and reluctantly stayed in the hands and knees position until her arms ached. Jennifer later admitted the rock (which was actually hard ground) was very uncomfortable. Meanwhile, David took to reorganizing the car and removing the extra towels from the bags and filling the flower vase with water from the Stephen’s Park water fountain that never turned off. Once he was done we realized it had been 5 hours since the last exam so it was time to check back in with the midwives. In thru the door of midwives' offices we went and down the hall where Jennifer traded her bottle of water for a bathroom key. In the bathroom, she moaned and groaned her way through a contraction so loud that the MD stopped in his tracks and with a look of concern but excitement asked if someone was laboring in there. We gathered in the exam room and the apprentice midwife, Karen, took a look at Jennifer and reported she was 4 cm, 75% effaced, -2 station. Since it had been 5 hours since the last exam we were all hoping things would be further along. Jennifer explained she was extremely tired after laboring all night. Karen massaged Jennifer through one contraction and then left the room to call Lisa who had gone home for a little bit. Karen returned and in so many words explained that the midwives were concerned because Jennifer's contractions were still not coming really strong and regular and they felt if the labor continued this way, it would go well into the next day with an extremely tired uterus. They suggested Jennifer get a shot of morphine to rest and after 2-3 hours start a low-drip pitocin. Jennifer and David were extremely reluctant to have any intervention. They imagined a natural birth, a waterbirth. Besides, Jennifer’s mom relayed stories from when Jennifer was born and there were details of intervention and screaming that Jennifer did not want to repeat. From Jennifer's perspective - intervention equaled bad experience. Friday afternoon 5p yay – mom is admitted to the hospital! The contractions were coming a little stronger now – “Aye carumba!! Jennifer yells. Karen met us and was saying a little sleep medication combined with oxytocin augmentation might help but Jennifer wanted to stick to her plan of no intervention. Karen tentatively started filling the bath to honor what Jennifer & David wanted but stopped a quarter way full. We were at a standstill until Lisa arrived. Karen got Jennifer into hands and knees position again to help reposition the baby. Lisa came in after about 20 minutes and saw the bath a quarter full, “what happened to the morphine shot in the butt?, and we informed her that Karen was going to let Jennifer try to do it the way she wanted,Lisa said “didn’t we already try that?” Lisa felt the labor was progressing too slowly and without augmentation Jennifer would still be laboring the next morning and she examined Jennifer herself. Another contraction, “Jesus Christ!” – Lisa says “I wouldn’t expect that out of you“ "I’m not Jewish! David is.” “Fuck!” followed by yogic ohms. Lisa finished her exam and then basically said this is what we are doing and Jennifer and David hesitantly agreed and in a matter of minutes the nurses had Jennifer hooked up to the EFM & IV, stuck her with the morphine in her right cheek butt (ouch!) and within 20 minutes Jennifer went from saying “this isn’t what I wanted!” and “I feel so restricted!” to “this feels good” and it feels “druggy.” About 10 minutes later, they started the pitocin at a very low drip, 2 ml. Pretty soon the room was like an oasis of scents and sounds. I put on some “insurgent country” girl Neko Case and David got the lavender aromatherapy pumping out from the diffuser. Jenn was trying to eat some snacks, like fruit roll ups and nuts and dried cherries. She had the talent of eating a fruit roll-up (organic of course) while in hands and knees position! David comforted Jennifer during the contractions while I rubbed her feet with peppermint foot rub and massaged her back with the lavender oil. Since baby was slightly occiput posterior she found it comforting when I applied pressure to her sacrum or applied a double hip squeeze during contractions. Our nurse kept a close eye on the monitor and levels. After a about 20 minutes, Jennifer or Dave fell asleep - I am not sure who but I heard the sound of snoring and deep breathing. I took the opportunity to eat dinner, which was a plate of spaghetti & meatballs we got from an extra tray left another mom didn't want. I ate half and saved the other half for Dave, who was also famished. Jennifer was still contracting during her sleep and when she did, Karen showed me how to rock her in the direction we wanted the baby to go. Also, the midwives administered pulsatilla, a homeopathic medicine to help reposition baby. I am still not clear how it works but the midwives seemed amazed that homeopathy works at all so I guess I am not alone in my wondering. The midwives returned a while later and when they came in they wrinkled their noses at all the smells, “eew I touched it" Lisa said when her fingers accidentally touched some essential oil. They probably have to be careful - imagine how scenty they would be if they dipped their fingers in the essential oils every time they went into a labor and delivery room! Unfortunately, everything Jennifer ate came back up. She vomited throughout labor and afterwards would always say - "that felt so good!" Jennifer also got the hiccups periodically. Lisa was very impressed with her hiccups and recounted one other mom's birth experience who also had the hiccups. I think it was around this time that she told us pregnant cats will seek out raspberry leaf to eat but it may have been another herb. Lisa brushed Jennifer’s hair to get it out of her face. Jennifer looked so beautiful I had to take a picture.  After the morphine wore off a bit and the pitocin was kicking in Jennifer got in the waterbath. The water provided some comfort - Jennifer tried different positions like squatting and lying to her side. The position that seemed to work the best was kneeling and burrowing her head into Dave and covering him with kisses. The contraction would came over her and she would burrow her head into Dave’s shoulders, sometimes pulling hair, sometimes digging her nails into his skin, and he reciprocated with kisses and nuzzles. Jenn found comfort giving and receiving affection and Dave was right there with her – even to the point of having scratches all over the back of his neck! I was really so amazed by how loving they were - kissing and hugging and nuzzling the entire time - and thought how reaffirming it is of the birth process that different women find different ways of coping during labor. I wondered if they are always that close or if birth brought them closer – probably a little of both. They were loving and sensual and supportive and such an exquisite example of what a mother and father can be. But then Dave let a coca-cola burp go right in Jenn’s face “ew gross! I am the only one allowed to do anything disgusting!” "I didn't mean to." Dave replied. This was a funny side because for the most part Jenn and Dave were totally loving and affectionate with one another. Jennifer continued laboring, when she was hot in tub I held an ice-cold cloth to her forehead and when she was cold we covered her in blankets. We could not do anything about Jennifer being wet from the waterbath but Nurse Karen didn’t seem concerned, "it is the same as if you stay in a wet bathing suit at the beach for 3 hours." Around 10 pm the midwives did another exam, Jennifer was 7-8 cm, almost 100%, thin lip. The exams always seem to get things moving so the next thing we know is Jennifer is experiencing a lot of bloody show while on the potty. The midwives were very happy about that because it meant things were moving along down there. They got Jennifer bouncing on the birth ball and within a few contractions her water broke, "that felt really good" Jennifer said. We were all tired at this point. Dave yawned but still let Jennifer dig her nails into him. Dave was tireless. Midwife Karen’s back was hurting – a pinched nerve or something - so the nurse fashioned an ice-backpack for her. Midwife Lisa was yawning and I think I saw her nod off for a second – sitting up no less! Quite a midwifery talent! I could not believe the midwives waited so patiently in the room the entire time - that is very unusual. And then there was Jennifer who expressed major discomfort at 2 cm but then here at 9 cm when we were all sleepy and dopey she was moaning her way thru every contraction like a champ. She found the resources within her. “oh God, God help me” she would say. Around 11 pm the nurse did her halfway thru the shift dance and by 11:30 pm all of us were there on the family birth bed. Earlier we were joking about who or why someone would use the birth bed but then there we were – all six of us! Jennifer had gone into the transition phase of you labor and the baby’s heart rate decelerated – Lisa said, "when the babies head gets mashed they don’t really like it” (when they enter the birth canal). It quickly returned to normal levels. They discussed bringing Jennifer back to the waterbath but were concerned to do so in case they had to get her out quickly. Jennifer was hoping for a waterbirth so they brought her back to the water and there she labored for a bit longer. I held her under her arms during the contractions and David sat beside Jennifer. Things started to seem more imminent because the LifeBank cordblood box and tools for labor came out. Maybe due to Jacob's position or some other reason, Jacob was taking his time and we still had a little ways to go. After about an hour, the midwives asked Jennifer to return to the bed. Since the 2nd stage was progressing so slowly the midwives were concerned there was a reason, either a tangled cord or shoulder dystocia, and wanted to be able to tend to whatever the scenario was quickly and efficiently if the need arose. So there we were on the bed again - Jennifer pushing. Dave put on a Matisyahu Cd to carry us into the midnight hour. When Dave got back on the bed, Jennifer said, “don’t shake the bed!" but that was about as abrupt as Jennifer got the entire night. I asked Jennifer to open her eyes and look at Dave's eyes so he could help focus her pushing and breathing. Counting seemed to help in terms of providing a beginning, middle and end to the contractions. After each contraction we’d have to slow your breathing down - “breathing in - one, two, three four five, and out” over and over again. They put an oxygen mask on Jennifer to get more oxygen to the baby. At first Jennifer didn’t want it and was concerned but then later would say, “oxygen is good.” At one point the midwives were concerned about the baby so they lowered the pitocin and the baby’s heartrate returned to normal once they made adjustment. The midwives were joking if Jennifer had the baby before midnight they could only stay two days whereas if the baby was born after midnight they could stay 3 days. Once the clock ticked past midnight Dave said “well the baby will definitely be born today.” We all thought that was hilarious and all piped in – “it had better be!,” what with 24 hours to go. Jennifer pushed and pushed through this very long 2nd stage. Eventually I just stood back and took pictures because Dave was helping with Jennifer’s breathing and only so many people can tell a mom to “push!” Apprentice Midwife Karen was standing ready to catch the baby with Lisa standing to her side. The midwives played with a little tuft of the baby’s hair that was sticking out. We told Jennifer we could see the baby’s hair and that energized her for these last round of pushes. Then at 1:42 am Baby Jacob was born into this world, “my baby!!!” Jennifer elated, opening her arms to her new baby, letting all the anguish and pain of labor vanish into pure joy. And the look of Dave's face was of wonder and relief. Karen caught Jacob and bundled him up so quickly I hardly got a look at him. The funny thing is everyone was so excited to see him and hold him, that no one bothered to look at what sex he was! “Did you look? I didn’t look!” The midwives took a peek. “A boy!” Jennifer and Dave smothered him with kisses. He coughed and cried and within a few seconds was looking at his mommy and daddy – so cute and so alert. And we joked he talked more than his mommy! Dave cut the cord and a few minutes later, the midwives massaged Jennifer's uterus and the placenta was expelled. The midwives did their charts and left to get some much needed sleep. The nurse watched over Jennifer saying, “You are doing just what I need you to do – lie there and nurse your baby.” Then within minutes, both of Jennifer and David's families swooned in! Wearing lipstick and jersey granddaddy t-shirts and everything! They had a very supportive family and they were all very excited to see their first grandchild! It was such an honor to be present at Jacob’s birth. I was so moved how loving Jenn and Dave were with one another – kissing and hugging and nuzzling the entire time. In one sense it reminds us of how Jacob came to be but also what a beautiful bond the mother and father have with one another and how lucky Jacob is to be born into their world. Thank you Jennifer & David for letting me witness the miracle of Jacob’s birth! ~ Rachel Kwock CD(DONA) Birth Doula |




 RSS Feed
RSS Feed